|
11/11/2023 0 Comments Example of simple random sampling
This creates a seemingly paradoxical situation in which higher levels of sample pooling often leads to prevalence estimates that are more accurate. A problem with imperfect specificity tests are that false positives typically outnumber true positives when the true prevalence is low. This could theoretically occur from PCR cross-reactivity between COVID-19 and other viruses, or from human errors in the lab. The situation changes when the test specificity ( θ) is set to 0.99, that is, allowing for false positive test results (Figs. 145 reactions is enough to get patient-level diagnosis 97.5% of the time, in other words a reduction in the number of separate RT-PCR setups by a factor of 34.5. However, sample pooling has been successfully used for seroprevalence studies for other diseases such as human immunodeficiency virus (HIV). Note that I will not discuss pooling of SARS-CoV-2 antibody-based tests, since there is currently not enough information about how pooling affects test parameters. 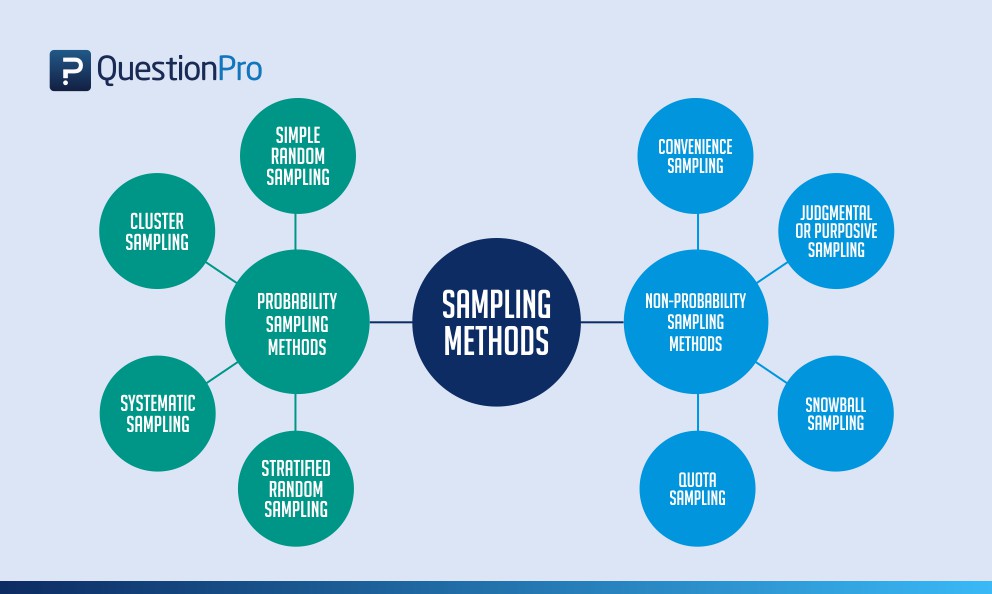
For SARS-CoV-2 pooling has been estimated to potentially reduce costs by 69%, use ten-fold fewer tests and clearing 20 times the number of people from isolation with the same number of tests. Pooling strategies, also called group testing, effectively increase the test capacity and reduces the required number of RT-PCR-based tests. Under such situations it can be advantageous to pool individual patient samples into a single pool. However, if the disease prevalence is low, very little information is garnered from each individual test. It is therefore possible to test randomly selected individuals to estimate the true disease prevalence in a population. 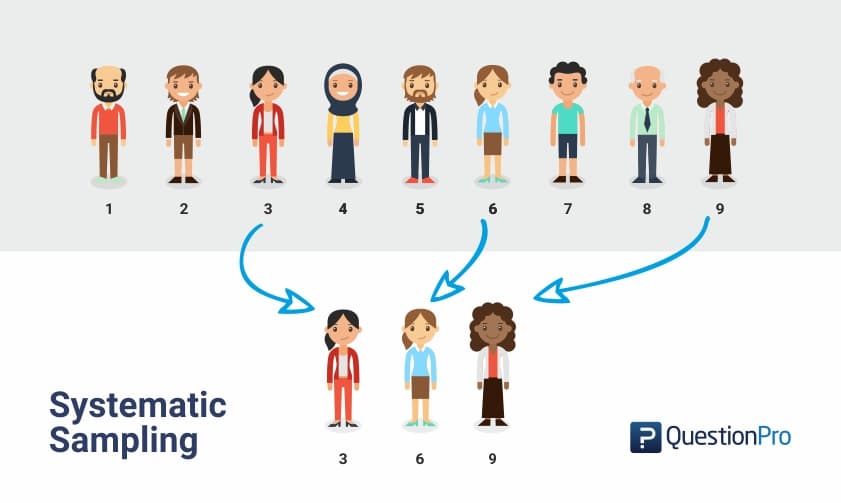
Non-symptomatic infections can still shed the Severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) virus and are therefore detectable by reverse transcriptase polymerase chain reaction (RT-PCR)-based tests. However, this is subject to large ascertainment bias since tests are typically only ordered from symptomatic cases, whereas a large proportion of infected might show little to no symptoms. A crude measure of population prevalence is the fraction of positive tests at any given date. It is widely accepted that a large fraction of COVID-19 cases go undetected. Sample pooling should be considered in COVID-19 prevalence estimation efforts. Sample pooling can be particularly beneficial when the test has imperfect specificity by providing more accurate estimates of the prevalence than an equal number of individual-level tests. Even when the true prevalence is as high as 10% it can be appropriate to pool up to 15 samples. In low-prevalence populations, it is theoretically possible to pool hundreds of samples with only marginal loss of precision. Sample pooling can greatly reduce the total number of tests required for prevalence estimation. Here I use simulations to explore how experiment sample size and degrees of sample pooling impact precision of prevalence estimates and potential for minimizing the total number of tests required to get individual-level diagnostic results. MethodsĮstimates of the true prevalence of COVID-19 in a population can be made by random sampling and pooling of RT-PCR tests. However, this fraction depends heavily on the sampling intensity and the various test criteria used in different jurisdictions, and many sources indicate that a large fraction of cases tend to go undetected. 
The number of confirmed COVID-19 cases divided by population size is used as a coarse measurement for the burden of disease in a population.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
